Editor’s note: This article was originally published by The Lund Report, an independent nonprofit news site covering health in Oregon.
For Joelle White, the worst part of watching her daughter go through fentanyl withdrawal was the uncontrollable screaming.
“You try to hold them, and they can’t be touched because their skin is crawling,” White said. “Everything hurts.”
Her 25-year-old daughter — whose name The Lund Report is withholding — has withstood the excruciating pain of withdrawal, the first step toward recovery, several times.
But each time she fought through the sickness, the level of treatment she needed to complete her recovery was not available. White, who lives in Scappoose, said her daughter has since suffered a fentanyl overdose that left her with some brain damage.
The spread of powerful and deadly synthetic opioids and stimulants in Oregon’s illicit drug supply has made fixing deficiencies in the state’s addiction care system increasingly urgent — and it’s presenting service providers with new dilemmas that can be heart-breaking.
“I don’t really have words to describe how much fentanyl has changed what we do,” Dr. Jennifer Hartley, a medical director for Fora Health, told The Lund Report. Fentanyl is a powerful synthetic drug that’s driven the surge in Oregon’s drug-related deaths, which stood at 1,161 last year, according to federal data.

Patients sleep at the Hooper Detoxification Stabilization Center in Portland on March 14, 2023. At Hooper, doctors and nurses oversee the medical needs of patients as they go through alcohol and drug withdrawal — a critical first step toward recovery.
Emily Green/The Lund Report
A nonprofit, Fora Health operates a facility in Southeast Portland for withdrawal management, also known as detox, where patients receive medical care for their symptoms after they stop using drugs or alcohol. Such facilities are a critical gateway into recovery for people whose drug dependence has become debilitating. But Hartley and providers like her say the prolonged withdrawal periods and more severe mental health problems associated with newer, more potent synthetic drugs — along with the lack of treatment options — are making their jobs harder.
A glimpse into what the staff at detox facilities are faced with shows how the system is failing their clients — even as they’re begging for help.
The realities providers described pose a challenge to Portland city officials who contend that sanctioned camps on the horizon will “meaningfully connect” people to drug treatment. Already, thousands of people, the majority of them homeless, show up to detox facilities within the city each year only to be turned away because there aren’t enough beds. And those who do gain entry usually don’t get the assistance they need when they leave.
“Every single day, we discharge people with very substandard plans,” Hartley said. “It makes me feel horrible. It makes our entire staff feel horrible. It is just the worst thing in the world to have to discharge somebody who is asking for help to the street.”
Thousands turned away from detox
Seven people gathered on the sidewalk outside the Hooper Detoxification Stabilization Center in Portland at the crack of dawn on a Monday in late March. It was 32 degrees outside, but only half wore coats.
Hooper sits on a ridge above Interstate 5 across the river from downtown. The constant cacophonous rumble of morning commuters and the roar of diesel engines echoed up from the traffic below.
Hooper is Oregon’s largest withdrawal management facility, operating 55 beds.
As they arrived, people hoping to gain entry filled out paperwork on clipboards and took COVID tests. Then they waited. Several had black-ink face and neck tattoos, the kind you get in prison or on the street. Others had fresh-looking scabs on their faces and exposed wrists. Most were dazed, standing, hands in their pockets or clutching cigarettes, hunched over and swaying slowly, or shivering, as they stared at the ground.
One man, wearing black jeans and knit cap, shifted every couple of minutes between slumping against the side of the concrete building and laying in the fetal position on the sidewalk. He was sick, in the early stages of withdrawal. Eventually, he threw up into a bag, his vomit matched the orange soda he’d been drinking. Sweat dripped from the tip of his nose as he threw the bag into a nearby trash can. The group slowly grew in number over the next hour.
At 8 a.m., a Hooper staff member began to call names. Fifteen people had showed up this morning.
It was “light for a Monday,” said Sarah Spofford, Hooper’s operations director. The Friday before, Hooper had to turn eight people away.
But on this day, twelve would be admitted promptly; two were told to come back in the afternoon. One was told to come back again tomorrow. Chances are that he won’t. According to Hooper’s internal data, only about a third do.
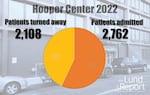
Source: Internal data from the Hooper Detoxification Stabilization Center, Oregon’s largest withdrawal management facility, located in Portland.
Lund Report
Last year, just over 2,700 people were admitted into Hooper’s inpatient withdrawal management program. Another 2,100 were turned away. It’s a staggering number, and it’s a number that Spofford said she hates.
A shortage of detox availability is a statewide problem. According to Oregon Health Authority data, on paper there are 308 licensed withdrawal management beds across the state. But some of those beds are out of service due to staffing shortages, and some of the facilities accept only private insurance — not government insurance, which covers a much greater portion of the people in need.
Of Oregon’s 36 counties, 28 have no withdrawal management services. The situation is worse than decision-makers and the public have been told. A recent, well-publicized analysis from the OHSU-PSU School of Public Health indicated that the supply of facilities was 27% short of what is needed. A lead author of the study, however, confirmed to The Lund Report that researchers mistakenly said detox services existed in two counties that actually have none.
For patients contending with alcohol withdrawal — which is more than half of the patients who enter Hooper — an inability to access medical care to oversee the process can be deadly due to the risk of seizure. People withdrawing from benzodiazepines — such as Valium, Xanax and Klonopin — face the same risk, Spofford said. But these patients aren’t necessarily prioritized for entry.
State regulations require that intravenous drug users and pregnant women be prioritized, though according to Hooper staff, if the patient has a history of seizures and appears in severe withdrawal, they will likely be admitted.
In 2020, Oregon voters approved Measure 110, which decriminalized possession of hard drugs and diverted hundreds of millions in marijuana tax dollars to fund addiction services. Its spending since then has focused on peer services, harm reduction, housing and other services. But it did provide funding for a sobering center in Grants Pass.
It also funded withdrawal management services in two other two locations. Washington County received $5.1 million for a one-stop recovery center that is supposed to include detox, though the project’s manager said the county still needs another $8.7 million to cover capital costs before the project can move forward. Providence Portland Medical Center received $3.7 million to set up an eight-bed sobering and stabilization unit for highly intoxicated patients admitted to the hospital.
Still, recovery service providers across the state — from Clatsop County on the coast to Malheur County on the Idaho border — told The Lund Report they have had to send patients to Hooper in Portland for withdrawal management.
But then at Hooper, “we just can’t meet the need,” Spofford said.
No next step
For a person caught-up in addiction, simply getting to a detox’s door for admission is a notable feat, providers say. Adding to the challenge, more than half the clients at Hooper and Fora Health’s detox are unhoused.
Once inside, it doesn’t get much easier. At Hooper, after a staffer runs through the rules with the new group of entrants, they have to wait as they cycle through intake: a medical screening, an addiction assessment and a shower. Sleep deprived or nauseous in many cases, they’re offered mats on the floor of a dark room where a TV flickers so they can lay down so the time passes less painfully.
Patients typically stay in one of two large, shared rooms, depending on their gender identity. Small partitions separate the beds, which are just feet apart. Approaching lunch time, these rooms were dim and quiet. Most patients slept. They will spend most of their time at Hooper in their bed, where they sleep and take their meals.
A team of doctors and nurses keeps a close eye as patients go through withdrawal symptoms that are often intense. They provide medications to ease pain and nausea, and keep an eye on vitals.

The Hooper Detoxification Stabilization Center is one of two drug and alcohol withdrawal management facilities in Portland.
Emily Green/Lund Report
While alcohol withdrawal can be life-threatening, opioid withdrawal feels like it is. The pain is so excruciating that without help managing it, people often relapse. Even with help, 1 in 5 patients leave Hooper before they’re stabilized.
About a third of Hooper’s patients will come back to go through withdrawal there again. Fewer would return if they got the help they needed when they’re discharged, said Dr. Andrew Mendenhall, president and CEO of Central City Concern, the homeless services nonprofit that runs Hooper.
He said before his nonprofit would expand detox, there needs to be somewhere to send patients afterward. Since the start of 2020, only 11% of people discharged from Hooper have been placed in residential treatment.
“If we’re going to have more medical withdrawal management, we need more residential treatment beds,” Mendenhall said. “We need more outpatient treatment capacity, along with stabilization, transitional housing services for those individuals.”
About 8% of Hooper’s patients are discharged to a homeless shelter, with a referral to outpatient treatment.
“We’ve had to place far more people into shelters post-treatment than we ever have in other years that I’ve been here,” Spofford said. And some go straight to shelters that house people actively using drugs, she said.
Hooper sends a quarter of its patients straight to housing after detox, because it’s more accessible than treatment. That housing may come with outpatient treatment, life skills training or other support, but really, Spofford said, patients often need residential treatment first to be successful at that lower level of care.
Fora Health operates the only other withdrawal facility in Portland. It’s licensed for 24 beds, though it couldn’t staff for that capacity during the pandemic, Hartley said.
She said every day, her staff hears from people that they cannot stop using drugs if they are living outside.
“They become so upset when they hear they’re not getting a bed in residential treatment that they just leave,” Hartley said.
Worsening psychosis and heightened needs
In the past, people who use meth typically benefitted from having a secure place to sleep, comfort medication and the connection to services that a place like Hooper provides, said Spofford. They might stay a couple days.
“But recently, as our meth has changed,” she said, “folks are having much higher levels of psychosis and more acute mental health symptoms in general related to their meth use, so people are needing more time.”
If a person shows up in severe psychosis, Hooper might send them to the Unity Center for Behavioral Health to be stabilized, after which Hooper takes over their withdrawal management.
“But now,” Spofford said, “there’s a higher number of them, and a lot more folks are declining going to Unity, so then they just leave treatment.”
At Fora Health’s facility, Hartley said fentanyl usage surged in the spring of 2021, and it has complicated her work.
“That’s when we really saw things start to change,” she said. She said staff uses medications to treat opiate withdrawals that they never needed before, and they have to use higher doses.
“People’s withdrawals can be much more severe — we have to send more people to the hospital for stabilization, because we can’t manage their withdrawal here,” she said. And when they stay, she said, some patients’ physical and mental health symptoms last longer after they come off medication.
When they no longer require the level of care her facility provides, Hartley said, “they are needing services that don’t really exist right now for post-acute stabilization.”
Providers often rely on buprenorphine to aid in opioid withdrawal, but with fentanyl, methadone is often a better choice. It can be administered right away, reducing the suffering involved.
Both Fora Health and Hooper are seeking federal permission to administer methadone.
But in the meantime, said Dr. Mike Winer, Hooper’s associate medical director, “it just makes it really hard for our patients, and it’s hard for us to kind of watch this and not be able to do evidence-based care.”
When housing isn’t enough
Solara Salazar sees another side of the same problem. She oversees six sober houses in the Portland area in her role as the co-founder and director of West Coast Housing. Her houses offer communal living to people willing to pass drug tests and participate in some level of recovery programming outside the home.
Some proponents of Measure 110 point to housing paired with outpatient treatment — two funding priorities of the measure — as a viable alternative to residential treatment. And for some people, it works.
But only about 10% of people coming to Salazar’s houses straight from detox are successful, she said. She defines success as someone staying for 60 days without leaving or relapsing.
And if they’re using fentanyl?
“We have had no successful clients who came directly from detox with fentanyl as their drug of choice,” she said.
Those tenants, she said, often come to her with fentanyl still working its way out of their system, even after being discharged from a withdrawal management facility.
“We are getting people that are still actively in withdrawal and are still detoxing and are sick and sweaty and have insane cravings,” Salazar said. She recently sent one woman back to a medical facility for continued observation.
This increases the risk of a person relapsing. And while any opioid relapse can be fatal, that risk is greater with fentanyl.
“We’ve had countless clients that were in our care, that are no longer with us, that have overdosed and died,” Salazar said. “And we work primarily with young adults, so these are 20-year olds — 25, 26 — like really young, and it’s really, really heartbreaking.”
One year ago, nearly 90% of her residents reached the 60-day benchmark. She didn’t have any residents then who primarily used fentanyl back then, she said. Now, the success rate has plummeted to 40%. And about a third of her tenants now say fentanyl is their drug of choice.
Also contributing to the declining success rate, she said, is that fewer of her tenants are coming to her from residential treatment.
“Everybody’s using fentanyl now, and so we have these people that really need a higher level of care prior to coming to sober housing,” she said. “And they’re not successful because we don’t have enough structure and services and resources that are needed. And that’s no fault of ours or the clients, it’s just this huge gap in residential (treatment) services.”
The gap is one that White, the mother in Scappoose, knows well. She blames her young daughter’s continuing downward spiral on her inability to get into residential treatment. A once “beautiful” and gifted artist, her daughter was “planning her future” after graduating high school, White said, but also had a list of mental health diagnoses that included bipolar disorder and autism. When the young woman was introduced to hard drugs, her fall into debilitating addiction and homelessness was swift.
After the first time she completed detox at Hooper, when she was 23, she was offered a bed in a sober house for women. It would be the only time she was offered a bed of any sort after detox.
Her mother remembers helping her clean up the tiny room that barely fit a twin bed and a dresser. Her parents would pay the $400 monthly rent while she looked for a job at a nearby fast food restaurant.
“She was excited, thinking that this would be a great transition,” White said.
But her daughter soon returned to the streets. She needed the structure and support of residential treatment, not sober housing, White said.
“There is nothing after detox. Everything is full. And the waiting list is a good month to two months out. And if you’re an addict, you can’t wait,” she said.
White’s daughter is still using drugs, but is no longer interested in help. “She tells me everything is too hard for her,” White said.
Treatment bed questions unanswered
Oregon officials say they are trying to address the lack of treatment services, but progress has been slow and hampered by workforce shortages and bureaucracy. And progress can be hard to measure.
Recent investments in behavioral health from the 2021 Legislature resulted in additional housing for people struggling with addiction, about 300 new beds. But it’s unclear what progress is being made in funding additional treatment beds.
There are 1,370 residential treatment beds for substance use disorder licensed in Oregon, though not all are necessarily in operation, according to the Oregon Health Authority.
Asked how many new treatment beds would result from the Legislature’s 2021 spending, spokespeople for the Oregon Health Authority and Gov. Tina Kotek said they do not know. They also couldn’t say how many treatment beds would be created under the governor’s proposed budget or the modified version crafted by the Legislature’s budget-writers in the Joint Ways & Means Committee.
Also unknown? The number of beds, treatment or otherwise, created with Measure 110 spending, as the state does not require grant recipients to report that.
What is known is that many more beds are needed. Rep. Rob Nosse, D-Portland, introduced a blank appropriations bill this session intended to put more funding into residential treatment, as well as other needs.
“We all know how desperate our state needs more treatment beds,” he told the House Behavioral Health and Health Care Committee in March. “We have some shovel ready projects, we have some that have applied for grants, and we simply don’t have the funds for them to break ground, and meanwhile, we need to make an investment.”
When the system works
Jon Mroz, 42, was one of the lucky ones.
Nearly two years ago, he was in a “wretched state,” he said, hobbling around downtown Portland in the midst of a stimulant-induced psychosis. He was homeless and his leg was broken, in a brace. He was shirtless, and he was yelling.
“I remember the psychosis, like, really vividly,” he said. “And I remember the fear, I remember just the nightmare of it all.”

Jonathan Mroz in Old Town on April 5, 2023, standing on the patch of sidewalk where he was living in tent before he entered a withdrawal management facility two years ago. Today he works just blocks away as a communications specialist for Central City Concern.
Emily Green/Lund Report
Passersby wouldn’t have guessed that the man screaming “liberty or death” as he staggered along the sidewalk was once an adjunct sociology professor at Joint Special Operations University in Florida, or that he authored policy papers for a New York think tank.
“I had a pretty good life, for a long time,” he said. He had issues with alcohol, he said, but for years remained “a functioning addict.”
But in 2018, his daughter and her mother moved to Portland, leaving him in California, where he had just taken a job in Long Beach. He was depressed. That’s when a neighbor introduced him to meth.
“Six months later, my life was up in smoke,” he said.
Eventually he came to Portland to be near his daughter, but he ended up living outside, enthralled in his addiction — which now included heroin — instead. He was sitting in a tent in Old Town on Aug. 19, 2021 when he “had this realization that I was going to die, and that this is what my life had been reduced to.”
He walked over to the Burnside Bridge with the intention of jumping off it but stopped. Mroz, who is Muslim, said that his higher power intervened and said “This isn’t how your daughter is going to remember you.”
He’d been to Hooper before but left before completing treatment. He made his way there again. He stayed in the doorway that night and applied for a bed the next morning. It was a Friday. There were more applicants than beds, and he was turned away.
Feeling angry, “I went out and got loaded,” he recalled.
The following Sunday, he set out for Hooper. He hadn’t slept in days and remembers wandering in circles for hours among the blocks surrounding the building, trying to find it. He eventually did, and stayed out front overnight again, praying all night that he would be admitted.
He got in, and he slept for three days. At discharge, he was connected to Central City Concern’s seven-month permanent supportive housing program and enrolled in intensive outpatient substance use disorder and mental health treatment programs at the Native American Rehabilitation Association.
The psychological rehabilitation was the hardest part. “It took a long time, it took a lot of therapy,” he said. “just getting over the psychosis of using methamphetamine was, like, really hard.”
Since then he’s remained drug-free. Central City Concern gave him a job “cleaning toilets,” he said, but he’s been promoted three times.
Now, he’s an internal communications specialist for the nonprofit. His office is just two blocks from his last campsite. And, in April, a judge granted him visitation with his daughter.
Mroz believes it was divine intervention that brought him back to Hooper when there would be housing and treatment available on the day he got out.
“That saved my life,” he said.
Emily Green can be reached at emily@thelundreport.org.