Oregon quietly reached a monumental milestone last week in the fight against COVID-19.
First doses of the vaccine for COVID-19 have reached almost every nursing home, assisted living and memory care facility in the state, according to the pharmacies distributing it.
But it’s still hard to evaluate how successful the effort has been: Getting the shot is voluntary, and the state has yet to release data on vaccination rates for residents and staff in long term care.
Phil Fogg, the CEO of Marquis Companies, a health care firm that owns one of the largest chains of nursing home and physical rehabilitation facilities in Oregon, calls the vaccine a salvation.
“This is what’s going to get us out of this nightmare of the last 12 months,” he said.
To sum up that nightmare too briefly: Nursing homes and assisted living facilities have been under tight regulations for almost a year, frequently closed to visitors, including family. That’s left residents struggling with the impact of extreme isolation over long periods of time.
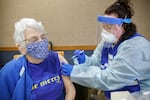
Margene Haworth, left, receives a COVID-19 vaccination from McMinnville paramedic Elle Miller, Feb. 5, 2021 at Friendsview Retirement Community in Newberg, Ore.
Kristyna Wentz-Graff / OPB
And the virus has reached these vulnerable populations anyway. About half the people in Oregon who have died of COVID-19 were sickened in an outbreak in long-term care or group senior living.
Early in the pandemic, an outbreak in a single Marquis facility in Canby sickened more than 100 people, and 18 died. Nine more people died in a second outbreak there this winter.
“The threat of this virus getting into a building, the threat alone, it just will drive you crazy,” Fogg said.
So Fogg threw his company into the effort to distribute the COVID-19 vaccine.
Marquis also owns a specialty pharmacy, Consonus, that manages medication for people in long-term care. It won approval to be part of the federal program delivering the vaccine to nursing homes and assisted living in Oregon and several other states, alongside pharmacy giants CVS and Walgreens.
A logistical maze
Oregon was one of the last states in the nation to open up vaccinations to the general population of seniors. But it was one of the first to start vaccinating in nursing homes, and it’s kept up the pace.
Last week, in data they publish online, CVS and Walgreens reported reaching every facility that was enrolled in Oregon with first doses of the vaccine.
Fogg says the process starts each day in a central pharmacy at 6 a.m. The Pfizer vaccine must be taken out of an ultra-cold storage container, nicknamed the pizza box, and then quickly repacked before it starts to thaw out.
“It’s like ‘Go,’ and you’ve got a clock, and you’ve got people pulling vials out and putting them into the different boxes that are going to different facilities that day, but they’ve got to do it in three minutes,” he aid.
Each long-term care facility in the state gets three clinics, three weeks apart for a first dose, a second dose, and then a make-up session.
“It’s kind of fun, to run the clinic. People are happy to be getting the shots. It’s not like going to the dentist,” said Vassar Byrd, CEO of Rose Villa Senior Living, a nonprofit retirement community and nursing home in Oak Grove. “It’s a community gathering in a weird way that people really appreciated.”

Vassar Byrd, CEO of Rose Villa, gives a thumbs-up as they await vaccinations to begin at the facility, Monday, Dec. 21, 2020. The facility says it was Oregon's first long term care facility to receive the vaccine. It has now vaccinated close to 100% of nursing home residents, and 85% of staff.
Kristyna Wentz-Graff / OPB
The vaccinations happened at people’s bedsides and in the performing arts auditorium. Thanks to a last minute waiver from the governor, some of the campus’s independent living seniors were vaccinated along with the nursing home residents. People wore masks and sat six feet apart. Byrd put out snacks from Mod Pizza.
It was the first time she was able to talk to residents in person since the pandemic began last March.
Rose Villa has completed all three of its vaccination clinics. The results: Almost 100% of nursing home residents got vaccinated, along with 85% of the staff.
Those rates are among the highest reported by any facility in the country, particularly for staff. Byrd says good communication and patience made the difference.
Some of Rose Villa’s staff waited to get their first dose.
“There were a few people who said, ‘I was nervous, but now I’m ready to go,’” Byrd said. “‘... We had no severe reactions at all to that first shot. So it made people feel just more comfortable.”
Months into the vaccination effort, it’s still hard to get a read on how comfortable staff at long-term care facilities in Oregon are with the vaccine.
OPB asked the Oregon Health Authority and the CDC what percentage of staff at long-term care facilities in Oregon have been vaccinated so far. Neither agency answered.
Vince Morr, a Brown University professor of health services, says that the average rate for staff, across facilities and states he’s looked at, is around 60%. Among residents, upwards of 80% have gotten the vaccine.
Morr is partnering with nursing homes on a randomized study testing a strategy to boost vaccine acceptance.
The study involves paying nursing homes to identify opinion leaders among their own staff: houeskeepers, maintenance staff, CNAs, and nurses. Then, researchers work with them to understand what attitudes or logistical problems are preventing staff from getting vaccinated, and to try to convince them its important.
“In spite of the bad rep nursing home workers get they really care about the people they spend 40 hours a week with,” Morr said. “Convincing them to keep their patients safe is, we’ve found, an effective strategy.”
What next?
Marquis has also reported promising rates of vaccine acceptance: 82% for staff and 90% for residents.
“We’re very very pleased with our consent rates,” said Fogg, the company CEO.
He believes there’s a generational difference in attitudes toward vaccines. Staff members are often younger and more likely to be fearful and need more information or education about the COVID-19 vaccine.
Residents, by contrast, are enthusiastic, he said. Many remember what the world was like before routine childhood immunizations.
“Between polio and smallpox and all the other things that they’ve done they’re not resistant to it at all,” he said.
With most residents in long-term care just weeks away from being fully vaccinated, it raises a big question: What comes next?
Fogg wants the state and the CDC to take a hard look at the restrictions on group activities and visitation that have left residents so isolated, particularly in facilities that have close to 100% of residents vaccinated.
“They need to be able to go to the dining room. They need to be able to socialize and be together. They need to be able to go to therapy in groups again,” Fogg said.
For visitation and group activities to start again safely, public health experts say vaccination for residents and staff is just one factor to consider.
Another key is driving down the rate of COVID-19 cases in the community. And to make that happen, it takes every Oregonian wearing a mask and practicing physical distancing.
