COVID-19 has now claimed 3,000 lives in Oregon. That figure was part of Friday’s troubling update on a pandemic that is overrunning Oregon’s hospitals, as the state recorded its fifth straight day with new cases exceeding the 2,000 mark.
State officials and those operating hospitals have an urgent message to Oregonians: if you are unvaccinated, stay home and avoid non-essential activities. If you are vaccinated, you should also take precautions — and avoid taking risks that could land you in the hospital.
It sounds a lot like what health officials were asking Oregonians to do when the pandemic began in March of 2020. But now, the situation in Oregon hospitals is much worse.
“Our health care system is on the verge of collapse in parts of the state. The numbers grow every day,” Oregon Health Authority Director Patrick Allen said.
There are 890 people in Oregon’s hospitals with confirmed or suspected COVID-19, about 300 more than have been hospitalized at any other point in this pandemic. It’s the first time Oregon’s hospitals have had to handle COVID-19 patient volumes like this.
The impacts of the COVID-19 pandemic on the health care system are widespread.
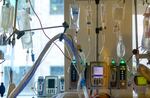
Every bed on this intensive care unit at Oregon Health and Science University is critically ill with COVID-19 in Portland, Ore., Aug. 19, 2021.
Kristyna Wentz-Graff / OPB
Hospitals around Oregon are starting their days with no intensive care unit beds available. And as of Wednesday, 93% of all the hospital beds in the state were full. That’s not even the entire picture.
At CHI Mercy Health Medical Center in Roseburg, doctors faced one of their biggest fears: a hospital so full that a patient died after waiting four hours for an ICU bed.
Emergency room doctors and nurses cared for him while they tried to find him staff and space.
Related: Inside OHSU’s fight to save the region’s sickest COVID-19 patients
“We’re asking ER doctors to step beyond their comfort zone and take care of some patients or conditions that normally would be in the critical care unit or the cardiac care unit. And it places everyone in a very difficult situation,” said Dr. Jason Gray, the hospital’s chief medical officer, in an interview with OPB’s “Think Out Loud.”
Usually, when hospital officials talk about available beds, they mean staffed beds. But at Providence Medford Medical Center, where some units are operating at 120% capacity. That’s so many people, according to Providence Medford Medical Center Chief Medical Officer Dr. Jason Kuhl, that “literally, we’re out of physical beds.”
At St. Charles Health System in Bend, there were 62 COVID-19 patients Thursday taking up about a third of its acute care beds. Oregon has fewer staffed hospital beds per person than most states, so there’s not a lot of room to expand capacity.
”These are beds that are being utilized for these very important patients with a severe infection. But [COVID-19 patients] are also taking the place of beds that are much needed for other care,” said Jeff Absalon, the president and CEO of St. Charles Health. “When you hear numbers about capacity, what I want you to know is, we are at or over capacity in our hospitals throughout the state.”
Those full hospitals have spillover effects. At Oregon Health & Sciences University in Portland, all four intensive care units were completely full.
System overload
This overloaded health care system has consequences for everyone, not just the unvaccinated.
Since the pandemic began, St. Charles has canceled or postponed over 3,000 scheduled surgeries.
”These are not cosmetic surgeries. These are patients that have cancer, heart disease, neurological disease, surgeries that are necessary to preserve life and function and they’re being delayed right now,” Absalon said.
Only patients with the most severe surgical needs are being seen, Absalon explained. “I don’t want to mince my words here: we are rationing care.”
Hospitals are so full that emergency departments are experiencing long wait times, bad enough that ambulances have to wait longer to get their patients in. And once patients are admitted to the emergency department, they could wait days for critical care beds to become available.
This is why Absalon is asking people to stop taking risks that could expose them to the coronavirus. And that doesn’t just mean avoiding crowded, maskless bars.
”What scares me the most about this is what’s been alluded to. If someone gets in an accident or has a heart attack or need for acute care, they might not get the care they need in a timely fashion,” Absalon said. “This is a time to really be cautious about your activities and keep yourself safe.”
Sending for reinforcements
On Aug. 13, Oregon Gov. Kate Brown announced the deployment of 1,500 National Guard troops to support frontline health care workers. The first 500 are being sent to hospitals in Deschutes, Douglas, Jackson, and Josephine counties, which have fewer resources, serve large areas and have been hard-hit by the virus. Some have already arrived.
“At this point, the National Guard is assisting with non-caregiver-type work,” Kuhl said.
Hospitals in Columbia, Curry and Marion counties and the Portland metro area will receive the next wave of Guard members.
Oregon has also requested almost 500 health care workers from other states — from nurses to respiratory technicians and is contracting with nursing crisis teams.
It will take weeks for much of this medical worker support to arrive, and hospitals are full right now.
On Aug. 11, Brown reinstated a mask mandate to combat the rising cases. But even as Oregonians take precautions, case numbers keep rising. And the people who get sick today may need hospital beds in the future.