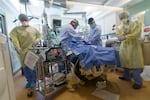
Staff prepare to perform a surgical procedure on the ICU floor. Every bed on this intensive care unit at Oregon Health and Science University was filled with a patient critically ill with COVID-19 in Portland, Ore., Aug. 19, 2021.
Kristyna Wentz-Graff / OPB
Two of Oregon’s biggest hospitals are reporting multi-million dollar financial losses, due to increased labor costs and other pandemic-related factors. Oregon Health and Science University is projecting an operating loss of $58 million for the 2022 fiscal year and St. Charles Health System has lost $21.8 million on its operations so far this year. St. Charles, which is the largest employer in Central Oregon, announced this week that it will lay off 105 employees. OHSU officials have said they hope to avoid layoffs and are looking for ways to increase revenue. We talk with John McConnell, director of the Center for Health Systems Effectiveness at OHSU about why hospital finances are so strained right now.
Note: The following transcript was created by a computer and edited by a volunteer.
Dave Miller: This is Think Out Loud on OPB, I’m Dave Miller. Two of Oregon’s biggest hospitals are reporting huge financial losses: St. Charles Health System, one of the largest employers in Central Oregon, has lost about $22 million so far this year. Oregon Health and Science University in Portland is projecting an operating loss of $58 million for this fiscal year. So what exactly is happening, and what does it mean for hospital staff and their patients? John McConnell is a health economist, and the director of the Center for Health System Effectiveness at OHSU. He joins us now with more details. John, welcome back.
John McConnell: Hi, thanks for having me on.
Miller: Thanks for joining us. Would you have predicted, say, a year and a half ago that hospitals would be losing money at this point?
McConnell: I did not see it coming quite this bad. It was sort of interesting, in the early parts of the pandemic, what we saw in the first two quarters, going back to 2020, was this huge dip leading to big negative margins, and then a rebound. Some of that rebound came from higher patient volume, and some of it came from payments from the government. And so my view in 2020 was that there was kind of an early hit and that things were going to look okay. So I think this caught everybody by surprise.
Miller: Things were going to be okay because people would be coming back to hospitals and getting colonoscopies and knee surgery and everything else. And my understanding is that people have been returning to hospitals. So, what are the challenges right now?
McConnell: I think there’s maybe three things and maybe maybe even a fourth that I’d point to. And so, what we’re talking about here is the margins are negative, which means that hospitals are losing money. And so those margins are your revenues minus your expenses.
People have been coming back, that happened a little bit, but there has been a drop in revenues. What’s happened, it looks like, is that with COVID, people stayed away. Some of them came back, but COVID hasn’t gone away, and it sort of changed the mix of services. And so for any hospital, some patients are more profitable than others, and some of these elective surgeries are more profitable than some of the emergency COVID -types of things. And it looks like some of the surgeries and elective surgeries are still down quite a bit, and that’s because the hospitals don’t have the capacity, and they’re seeing some of these COVID patients that are still coming in, hospitalizations for COVID are up again in Oregon. So, revenues have taken a big dip in 2022 and that wasn’t foreseen, that’s kind of the first one. Revenues are down.
And then expenses are way up. We’ve heard about workforce shortages and burnout, and healthcare has not been exempt from that. The cost of nursing has gone up a lot, I think people have heard a lot about that, but there have been other really big changes in expenses related to medical supplies. Prices of drugs are way up. As one example, people remember the name Remdesivir, that’s a drug for treating COVID once you’ve gotten it in the hospital. And that cost was initially covered by the federal government, but now hospitals are paying for it, and that’s kind of the top spending drug for hospitals.
And then the third is the way that the government support has played out for this. I think we all thought this would maybe last a year or two, and the CARES Act provided some funding for hospitals that got them through the first or second wave of the pandemic, and really created some space for them to have some positive margins during those first two periods. But that expired, so that’s no longer there. And then in some cases, hospitals are having to pay back some of that money. So there’s kind of a double whammy there.
So I think the combination of lower revenues is happening, especially among some of the bigger hospitals, they’re not seeing this increase in surgeries, really large increases in expenses, no more government support in some cases paying that back. And then I think a really uncertain environment in terms of what’s COVID doing and what’s the economy going to look like. That’s an X factor or that I would add there.
Miller: In the middle of the list you just mentioned, in terms of the reasons for higher costs, was labor? How exactly are labor issues connected right now to financial woes?
McConnell: Well, I think that the general cost of all labor has gone up. We know that there’s inflationary pressures. There’s been shortages of nurses nationwide. When you’ve got shortages, one way of responding to that is to pay higher wages. I think nationwide across hospitals, the cost of labor has gone up, especially for nurses.
Miller: What options do hospitals have when they are hemorrhaging money?
McConnell: Well, the simplest case is you can try and cut your costs, or you can try and increase your revenues. And I think we see different strategies both here at St Charles and at OHSU. So St Charles has announced some layoffs, and so they’re trying to respond by cutting some of their costs. OHSU is planning on sort of trying to keep its staffing as is, and hoping to grow revenues over a five year time period.
Miller: How do you grow revenues at a large hospital? What are the levers you can pull?
McConnell: Well, I think some of it is planned through increased patient volume. And so some of that may be expanding the market of patients that they serve, some of it may be expanding the services that they offer. There’s always new and different services that can be offered through different types of medical care that people need or want. And then some of it is sort of how you negotiate with insurers, and try to adjust either the payer mix that you have or the payment rates that you can get from private payers.
Miller: How much does a hospital have the ability to increase what it charges to insurers, and then trickling down, what it charges to patients? How much can actually increase costs?
McConnell: How much they can ask for higher rates is a good question. And I think it will depend on a few things. Some of it is the market power of the hospital. This is something that the state has been worried about, and it’s been a national trend, is concerns that, pre-COVID, certain hospital systems or certain provider groups were using market power to drive prices up. And that was a big contributor to increased prices that were a big concern pre-COVID. Everybody’s worried about the cost of health care. And so depending on how much of a monopoly a hospital has in its area, or how much of a big system it is part of, it may have some opportunities to negotiate for higher rates. That won’t be true for all hospitals, but could be true for some.
I think there will be kind of an interesting dynamic here in terms of how sympathetic insurers are to some of the increased costs there. And so that’s going to be negotiated. This is a new increase in costs that is a pretty different trajectory than what we’ve had over, say, the last decade. And so how that plays out through negotiations will be important.
And then there’s a third piece here, which is some new state legislature and the health care cost benchmark. This is a law that was passed somewhere in 2018 and the implementation began in 2019. And the idea here was, pre-COVID, one of the big concerns was the growth of healthcare spending. And so a few states, maybe five or so, have really tried to put some policies in place to try to observe and control healthcare spending. Oregon was one of the leaders here, and they have something called the healthcare cost benchmark. They brought together a variety of groups and tried to come up with something that they thought would be mutually agreeable and beneficial for the state. And the idea was that the healthcare spending they would try to target and limit it to 3.4% annual growth, and that sort of averaged out over a few years. That was all done pre-COVID, and I think that law is still in place, and I think the desire there is still to have healthcare spending be at 3.4% or lower. But it could be challenging. That was designed under a regime where the underlying cost trends for labor, drugs, supplies were not quite what we’re seeing today. So that’s gonna be another interesting dynamic that we’ll have to pay attention to.
Miller: You mentioned that broadly there are only two ways out of this for hospitals that are losing money as they operate. One is two reduce costs, the other is to bring in more revenue. I’m wondering, broadly, if the financial incentives are in place for overall community health to be the most important consideration. If a large hospital is going to maybe make more money on specialty care than on primary care, and if they need to make more money, then what happens to preventative care, and what happens to overall community health?
McConnell: Well, that is the $40,000 question. Are our payments aligned to really optimize population health? And I think in a lot of cases, they aren’t. I think that we know that, unfortunately the way payment goes right now, treatment of some types of conditions are pretty profitable. And if you’ve got big margins, you have to kind of play by the rules there. But we also know that there are certain areas, especially in the behavioral health realm, where we have a lot of excess suffering and deaths, and those conditions don’t pay as well as we might want them to.
So that’s a big question to end on here. But there are some concerns from economists and policymakers about whether the payment system is set up to really optimize patient health, and whether we have the incentives set up to really help hospitals and health systems find their way out of this, but also improve population health as we’re doing all of that.
Contact “Think Out Loud®”
If you’d like to comment on any of the topics in this show or suggest a topic of your own, please get in touch with us on Facebook or Twitter, send an email to thinkoutloud@opb.org, or you can leave a voicemail for us at 503-293-1983. The call-in phone number during the noon hour is 888-665-5865.
