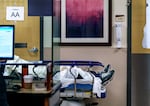
A patient waits for care in the hallway of the emergency department at Salem Health in Salem, Ore., Jan. 27, 2022, during the initial omicron surge.
Kristyna Wentz-Graff / OPB
Oregon will continue to see a rise in COVID-19 cases, along with hospitalizations and deaths, over the next few weeks. That’s according to Oregon Health & Science University data scientist Peter Graven.
The current surge is driven by the omicron subvariants BA.4 and BA.5, which are the most transmissible of the COVID-19 variants thus far in the pandemic. They’re also very good at evading immunity from vaccines and prior infections.
Graven’s forecast indicates that infection levels will likely be similar to what Oregon experienced with the first omicron wave in January.
Graven joined OPB’s “Think Out Loud” to talk about his latest forecast. The following transcript has been edited for clarity.
Dave Miller: The most dramatic spike in cases we saw in Oregon was around mid-January when omicron first took off here. But looking over your latest forecast, it seems like you’re predicting a similar spike later this month. Is that right?
Peter Graven: That’s right. We are back to really high infection levels. And while the case counts may seem a little bit lower this time — you may be seeing them around 1,700 a day — the infection levels that both the model is thinking and what we’re seeing in the wastewater are back up to those same levels we had back in January during the BA.1 subvariant wave.
Miller: Meaning as high as we’ve had in this entire pandemic. That’s what you’re expecting in the coming weeks?
Graven: Exactly. While we know we’re not catching all the cases, the infections that are out there we think are as high as 6% of the population. And that’s a similar level as we had before. So, if you’re if you’re hearing a lot of people around you look like they’re getting BA.4 and BA.5, which they won’t know, but they’ll have COVID, it’s true. We think those infection levels are really quite high right now.
Miller: What are you expecting to see in terms of hospitalizations, which for a long time was the most serious and important single number in terms of how as a society we are weathering any particular outbreak?
Graven: Here’s where we’ve seen a real change, and it started with the wave that began in January. We’re seeing less severity and more incidental hospitalizations across the state. That’s continued, and indeed while we’re having very high infection levels, I’m expecting our hospital census to only get up about half as high as it did in January. And again, within that, there’s a good share that are going to be incidental. What does that mean? That means you’re there for a broken leg or some other procedure where you happen to have COVID, but that may not be the main reason you were there. So when we look at those rates, we say, Well, actually with a really high infection level, we’re seeing not as many people needing the hospital urgently for COVID, which is probably the silver lining in this. We really have built up some immunity to those most severe outcomes that we’ve been trying to avoid.
Miller: Whether from prior infection or from vaccination and boosters?
Graven: That’s right, yeah. When we talk about immunity, it’s from either one — prior infection or vaccine. Now of course, I think we all know that the vaccine version is going to be easier to take. You’re less likely to get very sick. You might feel a little something the next day, but for the most part, you’re not going to get that illness where I think if you talk to people, you’ll hear that some people really are going to be sick for a number of days, maybe even up to the full 10 days that they indicate you could be sick for. And when we see that we say, well, if you’re looking at vaccines versus prior infection, you’re going to want to get your vaccines in as being your immunity builder. And those have helped, and we do see pretty good evidence now that as that builds up over time, your body tends to remember it, making it less likely that you get very sick.
Miller: But not necessarily likely that you’re not going to get sick at all. I mean, what are we learning about how quickly people can be re-infected, especially by one of these new variants?
Graven: It’s getting pretty quick. So, the reason why these subvariants exist is because they found a way to get past the previous immunity that you’ve had. So, even if you if you got the BA.1 or BA.2 — those were as recent as January or March or April — you could get re-infected with the BA.4 and BA.5. Now, it’s less likely than someone who hasn’t, but it’s certainly possible and we do see those reinfections. Usually, it doesn’t mean that it’s going to be more severe the next time you get it. So, we’re not seeing that sort of cascading problem, but it is certainly possible to get reinfected, and that’s something that we know that these variants want to do. They want to stay in the transmission in the population, and that’s what we’re seeing.
Miller: Can you give us a sense for just how contagious these newly dominant variants are — BA.4 and BA.5 — compared, say, to the very first virus that emerged out of Wuhan or other ones that followed — delta or others?
Graven: Yeah. So you know we measure that through a metric called the R0 (”R naught”) and so as the number gets higher, it means it’s more transmissible and it basically measures how many people you infect on average and that, of course, means that it’s finding ways to get into others. The original virus had an R0 of about three, which means, on average, each person infected will infect three others. The current version is around eight in my model. Different people use different parameters, but as you can see, that’s basically three times as transmissible as the original. And so it’s going to find a way. Certainly, indoor settings are very easy for this to transmit, certainly without a mask on, and even with a mask we’re seeing that it needs to be a better-fitting mask in order to really feel comfortable to not get the virus indoors.
Miller: The FDA has called for booster shots that specifically target BA.4 and BA.5. What do you say to people who might be waiting for those rather than getting their boosters now?
Graven: I would say that it’s probably not a good strategy to try to out-think the virus. I can tell you just from a forecasting perspective, you really never know what’s around the corner. And by the time these strains come, they come and go so quickly that would be really hard to prepare in advance for something that you don’t know that’s there. So quite frankly, I recommend a strategy of just getting the doses when you’re eligible. We know each one of those doses does help you. It’s incremental. It’s going to improve your chances and you’ll never know when the next one for sure is going to get you. So, I would recommend just getting them when they’re eligible. If a new one comes out, BA.4 or BA.5, that could be fall, could be late fall. We don’t know yet. So, I wouldn’t wait for it.
Contact “Think Out Loud®”
If you’d like to comment on any of the topics in this show, or suggest a topic of your own, please get in touch with us on Facebook or Twitter, send an email to thinkoutloud@opb.org, or you can leave a voicemail for us at 503-293-1983. The call-in phone number during the noon hour is 888-665-5865.
