Data from the Oregon Health Authority appears to show emerging racial and ethnic disparities in monkeypox cases.
People who identify as Hispanic account for 32 out of the state’s current total of 116 cases. That’s about 28 percent of all cases, in a state that is 14 percent Hispanic.
Black people and American Indians and Alaskan Natives are also overrepresented in the state’s monkeypox case count.
To date, the majority of all cases in the outbreak are occurring in gay and queer sexual networks; specifically in men who have sex with men. The risk to the general public is considered low.
The disparities mirror those seen in HIV cases in the United States.
The ethnic disparity in cases evokes the first year of the COVID-19 pandemic in Oregon when the Hispanic population had higher case, hospitalization, and death rates from COVID-19. Yet for months, Latinos had the lowest rates of vaccination against COVID-19, which many pointed to as a key failing of the state’s pandemic response.
Then, Gov. Kate Brown was slow to make agricultural and other service workers eligible for the vaccine, and a time-consuming online lottery system further excluded many who most needed the protection of the vaccine.
It’s difficult to say if Oregon is doing a better job of addressing the racial and ethnic disparities emerging in the monkeypox outbreak. The health authority did not have statewide data on the race or ethnicity of people who have been vaccinated to date.
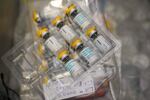
The monkeypox vaccine is seen inside a cooler during a vaccination clinic at the OASIS Wellness Center, Friday, Aug. 19, 2022, in New York.
Mary Altaffer / AP
Public health officials in Multnomah County, the center of the outbreak, did share their vaccination data. They have ethnicity information on about two-thirds of the 1,116 people who’ve been vaccinated at county public health clinics. And 17% of those people identified as Hispanic.
However, county officials noted that the very small number of cases so far and the dynamics of the monkeypox outbreak make it challenging to draw conclusions about racial and ethnic disparities. In part, that’s because the county doesn’t have any reliable estimate of the percent of white people or Hispanic people who are men who have sex with men, the group that is at highest risk and is eligible for vaccination.
However, public health officials in Multnomah County say given what the data is showing so far, they are targeting outreach and vaccines to Latino men.
“We do have some muscle memory from COVID,” said David Cuevas, a manager on the STD and HIV prevention team at Multnomah County Public Health.
The county has posted information in Spanish about the virus online and on social media. Staff is passing out information about the virus at bars and clubs that host Latino dance nights. Public health teams in Multnomah and Washington counties are meeting weekly with two dozen Latino community groups, to help with outreach and referrals for vaccine appointments. And the county is reserving a number of vaccine appointments specifically for Latino residents. Callers to the county’s call center who select the Spanish line or request an interpreter are prioritized.
Cuevas, who is a gay Latino man himself, says significant challenges remain, in particular overcoming the shame, fear, and confusion associated with a new virus that’s transmitted primarily through sex. Those feelings may make a person less likely to the doctor to get care, or to ask a family member for help, he said.
In addition, as the virus has become publicly associated with the LGBTQ community, people may fear that seeking help will out them as gay or queer.
“We have to be extremely careful about that,” Cuevas said.
That’s why, he says, it’s important to let people know that the virus can pass through skin-to-skin contact and that anyone can get it.
While it is primarily in gay and queer sexual and social networks, those networks are not self-contained and include people with other identities.
“Politicians and the media might care more about your identity, but the virus cares about the networks more than anybody’s identity,” Cuevas says. “It’s just looking for the next connected person.”
Cuevas said people who call the county’s call center to ask about the monkeypox vaccine will not need to discuss their sex lives in detail.
Instead, they can answer a simple ‘yes’ or ‘no’ to a series of questions that will determine whether they are eligible.
