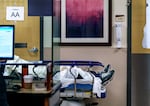
Gurneys line the hallway of the emergency department at Salem Health in Salem, Oregon, Jan. 27, 2022. The department has 100 patient beds including beds stationed in the emergency department hallways.
Kristyna Wentz-Graff / OPB
Mornings in the emergency department for the team at Salem Health’s Salem Hospital begin with quiet and anticipation.
Nurse Heather Gatchet’s shift typically starts at 6:00. She packs her daughter’s lunch, drinks tea, and calls her mom from the car.
“My mom’s like my cup of coffee” Gatchet said. “To mentally psych myself up for what I’m walking into, almost a little panic before I come to work.”
More than 700 days have passed since the first confirmed case of COVID-19 in Oregon. Deep into the second year of the pandemic, the hospital where Gatchet works is adapting, yet again, to try to accommodate more patients than it has licensed beds for.
The hospital has been above 100% capacity for months, with patients doubled up — and even occasionally tripled up — in their rooms.
On the phone, Gatchet’s mom encourages her. “You’ve been doing this a long time,” she says. “I love you.”
Gatchet clocks in and walks into the break room, and her panic lifts.
“This is my team and it feels safe again,” she said.

Salem Health clinical nurse Heather Gatchet says calling her mom before her morning shift at Salem Health hospital is part of her regular routine. “My mom’s like my cup of coffee” Gatchet said. “To mentally psych myself up for what I’m walking into, almost a little panic before I come to work.”
Kristyna Wentz-Graff / OPB
In a state where every hospital is buckling, Salem Hospital routinely treats more COVID-19 patients than any other. It’s the only hospital in one of Oregon’s larger cities, and the only major trauma center for miles. It has one of the busiest emergency departments on the West Coast.
As omicron has swept across Oregon, the managers here have decided not to go on what’s known as “divert,” a status that alerts ambulance drivers that an emergency department is full and patients should go somewhere else if possible.
That’s because every hospital in the Willamette Valley is basically full.
Dr. Peter Hakim works alongside Gatchet. Recently, his mother-in-law had a heart attack and was taken to a small, rural hospital. She needed specialty care that wasn’t available there.
“They could not find a bed for her anywhere in Washington or Oregon for 24 hours. So she was sitting in this small six-bed emergency department and couldn’t get transferred out,” Hakim said.
Hakim called a supervisor and tried to get his mother-in-law transferred. There wasn’t any space.
“At that point, I think our hospital capacity was about 115%. And we had 40 people waiting in our emergency department for beds upstairs,” he said.
His mother-in-law was lucky, and didn’t suffer due to the delay in getting her specialty care.
A lot of people, Hakim said “are not as lucky.”
“Just figure it out each day.”
The Salem Health hospital emergency department has 100 beds. To handle the influx of people seeking treatment, hospital staff have made space by putting dozens more beds in the halls.

Finding room to treat patients coming into the emergency department at Salem Health hospital has been a challenge, says Dr. Peter Hakim. The emergency department has 100 patient beds, including beds positioned in the hallways.
Kristyna Wentz-Graff / OPB
By noon, those hall beds start to fill up as patients fill the waiting room out in front of the emergency department and ambulances pull up to the bay behind the hospital… seven, eight, nine at a time.
The pressure builds through the afternoon as more patients arrive. By the evening, the hospital itself is full, and the hall beds in the emergency department are the only place left for new patients to go.
It’s hard for Gatchet to concentrate on the person in front of her amid the overwhelming noise of all the other patients.
“They’re crying because they’re in pain or they’re screaming because they’re having a psychiatric crisis, or we’ve put an alarm on them to alert us if they’re trying to climb off the gurney for safety reasons,” she said.
Three years ago, treating people in the hallways would have been an extraordinary measure. Now Gatchet and Hakim prepare for it every day.
Some of what Hakim does as a physician, like cutting off a patients’ clothing to examine a broken hip, is too sensitive for the hallway.
Some days, Hakim has a single room available and five or six patients who need urgent evaluation and some measure of privacy.
So he’ll move a person into the room, and then when he’s done with their exam, or he’s stabilized them, he’ll move the patient back out into the hall so he can treat the next person waiting.
Two weeks ago, Hakim evaluated a seriously ill patient in a bathroom.
“I have to see what’s going on,” he said. “And that is the one private space we could find at the time.”
A fragile system stretched beyond capacity
Last week, Salem Health broke its own pandemic record for COVID-19 patients — 122 people, nearly 1 out of every 4 patients in the hospital.
About 70% of that COVID-19 tally is patients admitted with respiratory symptoms, according to hospital executives. The other 30% are asymptomatic cases screened during admissions.

Nurse Camille Dickey enters the room of a COVID-19 patient on the medical-surgical unit at Salem Health, Jan. 27, 2022.
Kristyna Wentz-Graff / OPB
But those 122 patients are just part of the strain the pandemic has added to this hospital.
If you picture the health system as a line of dominoes, emergency medicine is at one end. But the domino that tipped first and knocked the other parts down is long-term care.
Statewide, more than 70% of long-term care facilities had a staff or resident COVID-19 case in January, with many reporting full-blown outbreaks.
Low-paid caregivers are burned out and quitting the long-term care sector in record numbers — one of many sectors competing for workers in a crunched labor market experiencing record resignations and retirements.
The outbreaks and staffing shortages mean that many places people go to recover after hospitalization are closed to new admissions.
It’s harder to find support too for patients who need assistance to return to their own homes after an illness or disabling accident. The pandemic has made hospital beds, in-home caregivers — even wheelchairs — all harder to get.
Dr. Sarah Webber, a hospitalist, says prior to the pandemic, coming up with a safe discharge plan for patients took her team a few days.

Dr. Sarah Webber, a hospitalist at Salem Health, says prior to the pandemic, coming up with a safe discharge plan for patients took her team a few days.Some hospitals are feeling the strain due to the recent surge of coronavirus, such as Salem Health, which had had 540 patients, but only 494 beds available on Jan. 27, 2022.
Kristyna Wentz-Graff / OPB
“And now sometimes is taking a week or two. And I do have some patients that have been here for several weeks,” she said.
Out of the 20 inpatients she was responsible for last week, eight were stable and ready to leave — but didn’t have a discharge plan.
Webber says people think of hospitals as safe places, but that’s an oversimplification.
The longer a patient stays, the more it increases the risk of infections, pneumonias, and becoming bedridden.
“It delays and potentially decreases a patient’s ability to become independent again,” she said.
Statewide, almost 600 patients are ready to leave the hospital but waiting on a discharge plan. One in 10 patients currently in an Oregon hospital bed could leave, but has nowhere to go.
The situation creates a vicious cycle: elderly or fragile patients never get the rehab or support they need to get stronger, and wind up back in the emergency department, where there’s little that physicians like Dr. Hakim can do for them.
“What they need is just somebody to stop by once or twice a day at their home to help,” Hakim said.
The COVID-19 Patients
As in the delta wave, a majority of the COVID-19 patients hospitalized at Salem Health are people who haven’t been vaccinated.
Patients infected with the omicron variant are, on the whole, requiring less oxygen and less intensive care.
“I’m seeing more patients live,” said Jackie Williams, a respiratory therapist who works on every floor of the hospital. “It’s like a little glimmer of hope, you know?”
Eight COVID-19 patients here are in intensive care beds, with just one ICU bed available.
There’s a contingency plan in place should the situation get even worse — to double up patients in the ICU.
But the hospital managers are relatively confident they won’t need to take that step.
Many of the less critical COVID-19 patients are behind closed doors in the hospital’s medical-surgical unit. The nurses here give patients oxygen with nose cannulas, turn them every two hours to prevent bedsores, and roll them onto their stomachs to help keep their lungs open.
But the sheer number of less critically ill patients is a struggle for the system to handle.
And even this seemingly milder form of COVID-19 is still devastating families.
In the hallway, a nurse manager speaks with the wife of a COVID-19 patient who’s been transferred from the emergency department.

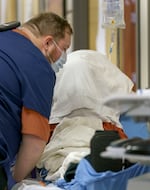
Nurse Camille Dickey dons PPE before taking a bag of clothing and glasses in to a COVID-19 patient.
Kristyna Wentz-Graff / OPB
The husband is behind a closed hospital door, on oxygen, with a warning sign on the front of his room so the nurses know to gown and mask before they go inside.
The manager is explaining that the patient’s wife needs to leave the unit, because she was exposed to COVID-19 while caring for her husband. The wife quietly fights back tears as she hands over a bag with glasses and a clean change of clothes.
“Does he have a cell phone? The nurses, they can help him do FaceTime so you can talk to him, okay?” The manager adds. “I’m sorry.”
The manager needs to protect her staff and all the other patients on this floor — people with diabetes and frostbite — against omicron infection. Even a mild case can put one of her nurses out of commission for five days.
“We’re already working with short staffing because of the surge,” she says.
An Oregon National Guard member deployed to the hospital to help out the nurses pushes a cart full of supplies down the hall and calls out a greeting.
The guard members provide a little lift — and a show of solidarity — to staff members who are feeling ground down.
For Dr. Sarah Webber, it stings that many of her patients still decline her advice to get vaccinated after they recover.
“People come to the hospital sick and they want me to help them, but they won’t trust me over the basics of how to help them or how to prevent it,” she said.
At home, she has less patience for her children — and they seem to need her more.
Her six-year-old daughter recently asked why Webber couldn’t just stay home with her.
“She asked me, ‘are the sick people more important than me?’” Webber said.
“I told her ‘of course not, they’re not more important’ and that I love her… but that those people also need me.”
Webber wants her daughter to see the value in public service.
“It’s a good thing for her to see that the world doesn’t revolve around her and that the world is full of sacrifice and putting others’ needs before your own.”
In just the last few days, hospitalizations in Oregon appear to have reached their peak — and are plateauing. The staff hope that as the omicron wave subsides, the pressure here will ease up a little bit.
Even if it does, it’s still flu season, the busy time of year.
The health system is as fragile as it’s ever been, and there will be another variant, another piece of the puzzle. The ambulances will keep coming. The waiting room will still be full. And health issues that have worsened through the pandemic in Oregon will resurface.
“It might not be breathing problems, but it’s alcoholism. It’s suicide. It’s traumas, it’s all these other things that are what the world is dealing with after coming out of two years of a pandemic and those are critical illnesses too,” said Jackie Williams, the respiratory therapist.
In the emergency department, Heather Gatchet does what she can to comfort the patients stuck in a place where the lights never turn off. They can’t see the smile underneath her mask, so she holds their hands.
“I’m trying to connect with people so badly,” she said.
“If I can help control their anxiety a little bit, maybe I can control my own energy and get through.”
At 6:00 pm, her 12-hour shift ends. She clocks out, gets in the car, and sings her heart out on the short drive home.