With 68.7% of Oregonians 18 and over vaccinated with at least one dose of a COVID-19 shot, less than 50,000 more people need to get a first dose for the state to reach the 70% target Gov. Kate Brown has set for a full economic reopening.
If vaccinations continue at their current pace, the state could hit that goal in a week or two — not by Gov. Brown’s original goal of June 21, but within President Biden’s national target for July 4th.
However, people running the vaccination effort for counties and health systems say while they’re confident Oregon will reach its target eventually, the rate of vaccinations has slowed to a crawl.
“We all expected it, but I don’t think we expected it to be that abrupt,” said Kim Toevs, who directs the COVID-19 vaccination program and case investigations for Multnomah County.
“We all of a sudden [had] saturated who was willing to do all the work and jump through the hoops and climb over the obstacles to get the vaccine.”
Two weeks ago, the average number of people getting their shot for the first time — primary doses of Pfizer and Moderna or a single-dose Johnson & Johnson vaccine — dipped to under 5,000 a day, according to data from Oregon’s vaccination registry published by the Oregon Health Authority. Statewide, most of the shots being administered are second doses.
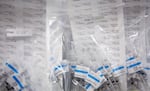
COVID-19 vaccine preparation at a drive-thru vaccination clinic at Portland International Airport, April 9, 2021.
Kristyna Wentz-Graff/ OPB
Additional OHA records show the rate of vaccinations has now fallen just below the most pessimistic projections the agency shared a month ago, when the governor set the 70% target for reopening.
The governor’s office isn’t yet clarifying what will happen if Oregon remains short of its vaccination target at the end of the month. Spokesperson Charles Boyle said the governor is “incredibly encouraged that over 2.3 million Oregonians have received at least a first COVID-19 vaccine dose so far,” and will be announcing later this week more details about what comes next.
Experts say 70% is no magic number, and health systems will need to continue the drive to try to increase vaccination rates statewide.
“I don’t think it’s oh, just a couple more weeks to get there,” said Katie Sharff, an infectious disease specialist with Kaiser Permanente.
“This is going to be an ongoing push and ongoing project through the rest of the year.”
The abrupt drop in new vaccinations poses a particularly sobering challenge for a handful of counties that have comparatively low vaccination rates and relatively large populations: Jackson, Douglas and Umatilla among them.
In Douglas County, a little more than 50% of adults 18 and up have received at least one dose of the vaccine, according to the county’s records.
Dr. Bob Dannenhoffer, the county public health administrator, says COVID-19 cases are continuing to spread among the unvaccinated people in his county.
“We’re still seeing lots of cases,” he said, “but now that 12 to 15 cases a day, rather than being spread over the whole population, is spread over the unvaccinated population. Which means that the attack rate for the unvaccinated is as high as it’s ever been.”
Three categories of unvaccinated Oregonians
Dannenhoffer in Douglas County and Toevs in Multnomah County agree that people who remain unvaccinated generally fall into one of three broad groups: people for whom the cost and inconvenience of making an appointment or visiting pharmacy is a barrier to vaccination, people who have specific concerns about side effects, and people who’ve decided they don’t want it.
Counties and health systems are deploying myriad strategies to try to make the vaccine more local and more mobile, in an effort to reach the first group: people who have no ideological bone to pick with the vaccine, but haven’t found a way to get it yet.
Conceding that navigating health system web sites is just too hard, they’ve moved to pop-up events and drop-in clinics with no appointments necessary.
In Douglas County, the health department has purchased an ATV-style vehicle it can use to take vaccines to fields to reach farmworkers who might not be able to forgo a day’s wages to visit a pharmacy. In an effort to reach new people, county public health workers brought doses to the Oregon Divisional Chainsaw Carving Championships in Reedsport Father’s Day weekend.
“We could be helped state and federally if it was easy to go ahead and a have a day off. Many of the people we’re talking about are people working in restaurants long and hard hours,” said Dannenhoffer.
Multnomah County has stepped up its vaccination outreach to people who are homeless and is working to make COVID-19 vaccines available through partners that run needle exchanges and health services sites.
Kaiser using algorithm to prioritize vaccine outreach
Kaiser Permanente has launched a pilot program that is even more targeted at getting the vaccine directly to people who need it the most.
The health system is using an algorithm developed by researchers at Oxford University, called QCovid, that uses factors like age, height, weight and ethnicity to predict an individual’s risk of being hospitalized or dying from COVID.
Kaiser is using the model to stratify its patients and identify those who are at highest risk, have been eligible for vaccination for a while, and aren’t yet vaccinated.
They get a call from a physician volunteer offering to have a conversation and help schedule a vaccination.
“A lot of these people have questions or concerns, and really just having that conversation about vaccinations and meet their patients where they’re at, it’s actually been quite successful,” said Katie Sharff, an infectious disease specialist at Kaiser Permanente.
Sharff says about half of the patients in the pilot have either scheduled their shot with the volunteer or said they plan to.
Helping people understand the importance of vaccination
Getting reliable information to people with concerns about side effects or the newness of the vaccine remains a heavy lift for health systems and health departments.
Meanwhile, vaccine misinformation is spreading rapidly on social media.
“There’s been so much misinformation on social media, lots of repeated rumors,” Toevs said. “Some of them feel almost malicious to me, in terms of their intention to drive people away from the vaccine, instead of letting folks make their own choice based on the science.”
For example, community health workers spotted a meme circulating among the Slavic community. It showed a close-up image of a needle bevel that had been photoshopped to make a tiny metal nanobot appear inside.
Toevs said she doesn’t know who is responsible for that particular image, but it’s part of a broader pattern of falsehoods about the vaccine on social media that are targeting specific immigrant communities.
“I don’t understand the motivation of people to do it,” Toevs said. “I’ve heard other people say, it’s pure racism or xenophobia.”
The myth that the vaccine can lower fertility, a falsehood that may have originated with anti-vaccine propagandists in Europe, is also prevalent online.
“On some of the social media platforms, you can be bombarded by information that seems really valid and real and perpetuates those myths,” Sharff said.
Toevs believes that for public health departments, countering the misinformation will require two key elements. First, continue to provide accurate scientific information about the vaccine, via trusted partners, in people’s native languages. And second, communicate respectfully with people who have doubts — including conveying the message that vaccination is a choice and the government won’t force anyone to get it.
Toevs has also stopped using the term “vaccine hesitant,” to describe people with concerns about the shot. It’s become a cliche.
“I think when we use a word over and over, it starts to paint its own picture,” she said. “And I think sometimes it helps to back off of that word and be a little more precise.”
The long game: “Be here, be available, be kind”
A third group of people has made a clear choice not to get vaccinated. For some people, not getting the shot may be a matter of identity, deeply held beliefs, or distrust of government.
Nationwide, about 20% of people said they would definitely not get the vaccine or will only get it if required, in May polling conducted by the Kaiser Family Foundation.
Health providers need to take the long view, and to listen without judgment when people say they have chosen not to get a COVID-19 shot.
Dannenhoffer, a pediatrician, says it’s akin to the approach he uses with parents who oppose early childhood vaccinations.
“What we’re trying to do is be here, be available, be kind,” he said.
“I’ve dealt with a lot of other vaccine hesitancy. With almost all those parents, we have this deal: We’ll talk about it, we’ll never make you feel bad about it, and when you’re ready for a vaccine, we’re here.”
