The recent on-the-job deaths of a Portland hospital security guard and a Gresham mental health aide have put a fresh spotlight on the violence that many working in health care experience routinely.
Some health care workers in Portland say they’ve been trying for years to get their employers and local politicians to do more to keep them safe.

Nurses and doctors from Providence Health, Legacy Health, OHSU, and the Portland VA joined a protest outside Legacy Good Samaritan Medical Center July 29, 2023. Health workers say they get too little support from managers and law enforcement when they are threatened by patients.
Amelia Templeton / OPB
Last weekend, a crowd of doctors, nurses and their family members marched outside Legacy Good Samaritan hospital in Northwest Portland. That’s where a security guard, Bobby Smallwood, was shot and killed in July. He was dealing with a patient and her partner who’d allegedly brought guns into the hospital’s family birth center.
The protesters gathered on a street corner and Jennifer Suarez, an emergency department nurse at Legacy Mount Hood, took the megaphone.
“Hitting, punching, being choked out,” she shouted. “You know, people saying they’re going to come back and blow our heads off. This happens on a daily basis.”
Suarez wore a backward baseball cap and a delicate gold nose ring. The organizers of the march passed out those red and white stickers with “hello, my name is” printed on them. Suarez, like many of the marchers, had filled hers in to read “assaulted.”
She told the crowd that nurses rarely get the support they need from managers to protect themselves.
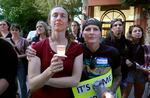
Nurses Bobbi Sue McColllum, left, and Jennifer Suarez at the candlelight vigil outside Legacy Good Samaritan Medical Center July 29, 2023. Suarez says too often nurses are told to accept being hit, kicked and threatened as part of their job.
Amelia Templeton / OPB
“We’re told, you don’t need to call the police for that,” she said into the megaphone. “They shouldn’t be trespassed for that… It’s part of your job.”
She paused, emotion filled her voice. “Dying or being assaulted is not part of our job!” she called out, to cheers from the crowd.
Smallwood’s death has struck a nerve among health care workers because many of them say while tragic, it did not feel surprising.
Homicides in hospitals are rare, but violence is not. Nurses and their assistants are regularly threatened, shoved, and punched by patients or patients’ family members. That’s not new. In 2018, for example, health care workers in the private sector filed more disability claims due to injuries from violence at work than people in every other private sector profession combined. Nationwide, 73% of all the reported workplace injuries due to violence happened in health care and social services.
But across the Portland metro area, health care workers say they’re now feeling less safe than they did even just a few years ago. At Oregon Health & Science University, nurses, through their union, have asked for more training in how to handle weapons they find on patients. And an outpatient clinic in southeast Portland recently closed for two days due to a bomb threat.
“I feel that people are so angry with the times and how the world is right now, they’re coming in so angry and so upset and they have a target to go right after us when we’re trying to help them,” said Tiffany Clendenin, an emergency department nurse at Legacy Salmon Creek in Vancouver, one of the protest’s organizers.
A patient in the emergency department threatened to kill her the day after Smallwood’s death. He was trying to leave the hospital with an IV still in his arm, Clendenin said.
“He just said, get away from me, you f-ing b, I’m going to f-ing kill you,” she said. Her tech tried to help her, but they got shoved by the patient too.
It’s not just nurses getting verbally and physically abused either.

Dr. Alex Skog, president of the Oregon chapter of the American College of Emergency Physicians, Aug. 2, 2023.
Kristyna Wentz-Graff / OPB
“Now, because there’s been so much politics mixed into health care, patients regularly doubt my motives,” said Dr. Alex Skog, an emergency department doctor and the president of the Oregon chapter of the American College of Emergency Physicians. “And I think that distrust is one of the main reasons we’re seeing this increase in violence.”
Another problem, according to Skog, who works for Providence Health and for the Portland VA, but does not speak for them, is that there are rarely consequences for hitting, kicking, or threatening hospital staff.
A patient can threaten staff, be escorted out by security, and then return the next day seeking care again. And legally, emergency department staff are still required to assess and stabilize them.
Skog says even when health care workers report assaults, it’s hard to get law enforcement to take action. Things like punching and kicking — assaults with no weapon involved — are generally misdemeanors. Prosecutors in Oregon rarely pursue those charges, Skog said.
A few months ago, Skog was punched by a patient who’d come to the Portland VA hospital for mental health care.
“I reported it to police,” Skog said. “They took notes, I followed up and I was told that charges weren’t gonna be filed on this patient. It’s not that I want to see harm come to other people, but I fear that if we continue down this path with no accountability for what might be considered mild assaults or just verbal threats, we’re gonna lead to more of these really serious incidents.”
Last year, the group of physicians Skog leads, Oregon ACEP, backed legislation that would have made it a felony in Oregon to assault hospital staff. The Legislature has done this for a few other professions: It’s an automatic felony to assault an EMT or a public transit driver behind the wheel.
Oregon’s powerful health care unions backed the bill, and it passed with bipartisan support in the Oregon House, though some Democrats said they were signing on to it very reluctantly. But it was never brought up for a vote in the Senate.
Two groups, Disability Rights Oregon and the Oregon Criminal Defense Lawyers Association, lobbied effectively against it. They gave examples of district attorneys who had filed misdemeanor charges against people who hit nurses and doctors. They argued that the people most likely to be prosecuted were patients who come to the hospital seeking help for a mental illness, and having a felony on their record could make it even harder for them to complete treatment or stay housed.
“We absolutely need to take care of our health care professionals,” wrote KC Lewis, managing attorney of the Mental Health Rights Project with Disability Rights Oregon. “But we cannot do it by furthering the harm we already inflict on those who are desperately seeking help for their mental illness.”
Skog said the bill may have applied to some people with a mental illness but it would have excluded anyone who was in active psychosis or couldn’t understand their own actions. He said he’s going to continue to bring the issue up with the Legislature. The issue continues to be an urgent one as hospitals continue to lose qualified workers, he said.
“I can’t say how regularly we’ve lost really good seasoned health care providers in the emergency department because they’ve just had enough of the way they’ve been treated over the last few years,” Skog said.

Bobby Smallwood's memorial in front of a security truck at Legacy Good Samaritan Medical Center on July 28, 2023. Smallwood was killed while working security for the hospital on July 22, 2023.
Caden Perry / OPB
Legacy Health has praised the staff at Good Samaritan in the wake of Smallwood’s death.
“Events like these are unpredictable, but our team exhibited professionalism and a great deal of courage in the face of extraordinarily challenging circumstances that day,” a Legacy Health spokesperson wrote in an emailed statement.
The health system has responded to the tragedy with a new security plan taking effect this month. It includes making metal detectors and bag searches the standard at every Legacy Hospital entrance, removing door stops so people can’t prop doors open, and providing stun guns to more of the security staff.
Sunita Patel is worried the new measures won’t be enough. Patel is a housekeeper at Legacy Emanuel hospital and a shop steward for SEIU Local 49, the union that represents housekeeping, certified nurse assistants and some other staff.
“And right now we feel really scared,” she said.
Patel has worked for Legacy Health for 19 years. She worked alongside Bobby Smallwood before he became a security guard, when they both staffed the front desk at Randall Children’s hospital.
“It really hurts me that he’s not with us anymore,” she said. She knew him to be a “really nice guy. [A] very kind, loving, gentle person.”
What concerns Patel the most is the threat of gun violence in the hospital and in the community that surrounds it. There are more frequent lockdowns now, she said, due to threats, due to people who have brought guns inside the hospital, or when there’s an incident nearby in the neighborhood.

Nurses join a protest outside Legacy Good Samaritan Medical Center in Portland as they get off shift from work. July 29, 2023.
Amelia Templeton / OPB
Patel says adding metal detectors at every entrance is a start, but it won’t be meaningful unless those metal detectors are staffed by security guards, 24/7.
“Like, we have a metal detector. We have two of them, in the two ED. Are they staffed 24 hours? Not really,” she said. “And we’ll continue to get hurt if we don’t start to fix this problem on safety and staffing.”
Legacy leaders say security is their top priority and that the health system has increased its investment in full-time security guards in recent years. Patel thinks they still need to hire more. We’re not just putting staff in danger, she said, we’re putting patients in danger too.
Correction: A previous version of this story misstated the Legacy Health employees represented by SEIU 49. That union represents housekeeping services, certified nurse assistants and some other staff.
