It's early morning in an operating theater at Providence Hospital in Portland. A middle-aged woman lies on the operating table, wrapped in blankets. Surgeons are about to cut out a cancerous growth in her stomach.
But first, anesthesiologist Dr. Brian Chesebro has to put her under. He starts by injecting one medication and then another into her IV.
“So here comes the one that’s really going to get you off to sleep. And this one stings sometimes,” Chesebro tells his patient, holding a mask over her face as she gradually loses consciousness. “Now I’m breathing for her with this mask, and I’m delivering sevoflurane to her through this breathing circuit.”
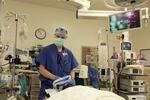
Dr. Brian Chesebro estimates that by using sevoflurance for this operation, he emitted the same greenhouse gasses as a 40 mile drive across greater Portland. If he’d used desflurane, he said, it would have been like driving from Seattle to San Diego.
Kristian Foden-Vencil / OPB
Sevoflurane is one of several gasses anesthesiologists use to put patients under. Desflurane is the other primary one.
Patients breathe in both the gasses but only metabolize about 5 percent. The rest is expelled into the hospital ventilation system and blown out the roof.
Sevoflurane and desflurane are similar and, up to now, anesthesiologists have tended to just pick one gas and stick with it unless there are medical reasons to change.
But as a doctor driven to dive deep on details, Chesebro researched them and found that desflurane is much worse for the environment than sevoflurane.

Dr. Michael Hartmeyer learned he could reduce his environmental footprint by changing from desflurane to sevoflurane. Dr. Chesebro figured the change was the equivalent of Hartmeyer going from driving 12 Hummers to half a Hummer.
Kristian Foden-Vencil / OPB
Not only is desflurane 20 times more potent a greenhouse gas than sevoflurane, but it also lasts for 14 years in the atmosphere. Sevoflurane breaks down in just one year.
"Part of growing up on a ranch is taking care of the land and being a good steward," he said. "And when I look around and I see stewardship on display today, it's discouraging."
His research led to a bit of a personal crisis: "I got depressed for a while, and so I hit the pause button on myself and said, 'Well, what's the very best that I can do?'"
Opening a big black notebook, filled with diagrams and tiny writing, he showed how the very best he could do was compute the greenhouse gas footprint of each of his fellow anesthesiologists. He shared those notes with them.
"All I'm doing is showing them their data," he said. "It's not really combative. It's demonstrative."
One of the doctors he showed was Dr. Michael Hartmeyer, who works at the Oregon Anesthesiology Group with Chesebro.
"I wish I had known earlier," Hartmeyer said. "I would have changed my practice a long time ago."
Hartmeyer says that when Chesebro explained that his use of desflurane was the greenhouse gas equivalent of driving a fleet of 12 Hummers, he was stunned. Hartmeyer drives a Prius.
Chesebro then told him that if he were to change to sevoflurane, it would be like only driving half a Hummer.
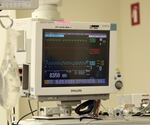
A vital signs monitor sits on top of an anesthesiology cart. The cart offers several different gasses. So an anesthesiologist can change gases relatively easily.
Kristian Foden-Vencil / OPB
“You try to be good. You take shorter showers or not leave lights on, or whatever else. But you know there’s always more that we could probably do," Hartmeyer said. "But this was, far and away, a relatively easy thing that I could do that made a huge impact."
The anesthesiology carts that get brought into operating theaters tend to have a row of gasses to choose from. So Hartmeyer was able to switch pretty much overnight.
Other anesthesiologists made the switch, too. It didn't hurt that sevoflurane is considerably cheaper than desflurane.
Hartmeyer's change saved his hospital $13,000 a year.
When Chesebro shared his findings with the anesthesia departments at all eight Providence Health hospitals in Oregon, they prioritized the use of sevoflurane. They now save about half a million dollars a year.
Providence's chief executive, Lisa Vance, said the hospital system didn't change because of the money. It changed because the World Health Organization now says climate change is the number one public health issue of the 21st century — and because of Chesebro. Vance said Chesebro teared up in front of 2,000 people when talking about the gas, his children and the Lorax from Dr. Seuss: "Unless someone like you, cares a whole awful lot. Nothing's going to get better, it's not."

A panel outside the operating room shows the levels of various gasses used.
Kristian Foden-Vencil / OPB
Jodi Sherman, an associate professor of anesthesiology at Yale School of Medicine, calls Chesebro's efforts remarkable and important.
She said several hospitals around the country have tried to make this shift but with mixed results. Some just gave anesthesiologists the information and not much changed. Other hospitals simply took desflurane away, but that left many anesthesiologists feeling disrespected and angry.
Sherman said she appreciates Chesebro’s commitment to giving his fellow doctors hard data on the impact their choices have on the environment.
“Providing ongoing reports to providers is the best way for this movement to catch on and grow,” she said. “It can reinforce over time both what the (carbon) footprint is but what the progress has been.”
Sherman said efforts such as Chesebro's are sorely needed because the U.S. health sector is responsible for about 10 percent of the nation's greenhouse gasses.
“We clinicians are very much focused on taking care of the patient in front of us," she said. "We tend to not think about what’s happening to the community health, public health, because we’re so focused on the patient in front of us."
In a statement, gas manufacturer Baxter Global says it's important to provide a range of options for patients. Baxter Global also said inhaled anesthetics have a climate impact of .01 percent of fossil fuels.
"The overall impact of anesthetic agents on global warming is low relative to other societal contributors, especially when you consider the critical role these products have in performing safe surgical procedures," read the statement.
It's a fair point, Chesebro said.

Dr. Brian Chesebro uses a large ledger to keep track of his research, just like his father, who was a scientist.
Kristian Foden-Vencil / OPB
“Desflurane is not a major player in climate change. That argument holds a lot of weight with a lot of people," he said. "My counter-argument is, 'Well, if it’s there, it’s bad. And if I can reduce my life’s footprint by a factor of six … why wouldn’t you do it?'”
The operation Chesebro was involved in that morning at Providence was a success. Chesebro estimates that by using sevoflurane on his patient, he emitted the same greenhouse gasses as a 40-mile drive across the Portland region.
If he’d used desflurane, he said, it would have been like driving from Seattle to San Diego.
Editor's note: A previous version of this story misidentified in a photo caption the gas that has less of an environmental impact.
