Earlier this week, Oregon Gov. Kate Brown announced she was extending a temporary measure aimed at not making the staffing crunch at health care facilities any worse. Brown approved a deal to keep 1,000 temporary contract workers deployed to the state’s hospitals, behavioral health programs and long term care facilities.
It’s just one measure of how short-staffed the state’s health care systems are.
Another demonstration of the problem comes from the stories nurses and other frontline workers are sharing about working conditions.

Julie Kleese, RN, cries after sharing her experiences as an ICU nurse at OHSU Hospital in Portland, Ore., Aug. 18, 2021.
Hanin Najjar / OPB
The number of COVID-19 cases and hospitalizations in Oregon has fallen significantly since September. A 64% decline in the weekly average of new cases was one of the statistics quoted by Oregon Health Authority director Patrick Allen when he announced the state’s decision to lift its outdoor mask mandate on Tuesday. At the same time, the working conditions for frontline medical workers have not meaningfully improved, as they continue to treat the patients hit hardest by the ongoing pandemic.
A number of nurses from around the state recently spoke to U.S. Sen. Jeff Merkley, D-Oregon, on a call organized by the nonprofit Oregon Center for Nursing.
Keith Coddington, a critical care charge nurse with the Asante hospital system in southern Oregon, described a work environment that has only gotten harder in recent months. Coddington said patients are sicker either because they have COVID-19, or because they delayed getting care. He said people who haven’t resigned are working unbelievably long hours.
“It is not uncommon in my critical care that I will have multiple nurses working that are on day 20 or day 21 straight of working 12-hour shifts,” Coddington said.
A nursing administrator at Asante responded that picking up extra shifts is voluntary and workers are paid overtime. She said Asante is not expecting people to work more than four or five shifts in a row.
But according to several health care workers familiar with the staffing issues, there’s also a work culture issue. Health care workers feel obligated to volunteer for shifts to help their colleagues, or they prefer working extra shifts than trusting the care of their patients to a temporary replacement.
Asante is trying to help by hiring traveling nurses, according to the nurse administrator, who said travelers are covering about 30% of the hospital’s hours. But that is a short-term solution to a long-term problem, and she’s concerned the situation only going to worsen in the next year.
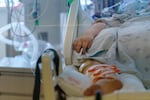
While COVID-19 cannot be cured—when people are hospitalized personnel are working to buy time for the patient’s body to heal. Every bed on this intensive care unit at Oregon Health and Science University is filled with a patient critically ill with COVID-19 in Portland, Ore., Aug. 19, 2021.
Kristyna Wentz-Graff / OPB
At the same time, health care workers have not recovered physically or emotionally from COVID-19′s toll over the last year and a half, including the surge over the summer. Hospital staff say people have left the workforce because they experienced too many deaths, or because they didn’t agree with vaccine mandates. Either way, that leaves patient care to a dwindling number of health care staff.
The problems are not unique to Asante in southern Oregon. Officials at the St. Charles Health System in Central Oregon said about 30% of their staffing positions are unfilled. That means other staff have to do more work, with nurses being responsible for more patients.
James Reedy, the chief nursing officer at St. Charles, said he’s had to have difficult discussions about what happens if there is another surge of COVID-19 patients and St. Charles lacks the staff available to treat them. In other words, they’re debating how to triage patients and provide palliative care only when there aren’t resources for every patient.
“Those have been some really just disturbing conversations that we’ve had to have,” Reedy said. “But it is, it is possible if we see another wave like this and don’t have the same resources available to us because people are exhausted in this marathon that doesn’t seem to end.”
The problems are also not unique to nurses. Merrick Barker, A respiratory therapist at Oregon Health & Science University in Portland, told OPB he’s worked shifts recently that have just half the appropriate staffing. Barker is not a nurse or doctor, but he has critical, specialized skills that allow him to help operate ventilators and provide breathing support to newborn infants, for example.
“We’re all burned out and exhausted, and money isn’t something that’s going to get us in the door any more when we’ve been so burned out and traumatized by what we’ve been made to see and do during that time,” Barker said.
He said he wants to work somewhere he feels heard and where his patients are safe.
Barker’s manager confirmed to OPB that some shifts, especially night shifts, have far fewer respiratory therapists than needed and that he sees and hears his staff’s distress. He’s heard concern about the level of care health workers can provide when they’re that short staffed.
